Doctors are trained to mass diagnose nearly everyone with depression (and put them on psychiatric drugs)
07/25/2018 / By Bridgette Wilcox

Health professionals will be the first to say that depression is a serious mental illness that must not be taken lightly — and yet it would appear that they themselves are guilty of doing so, relying only on a simple questionnaire created by a pharmaceutical company to arrive at a diagnosis.
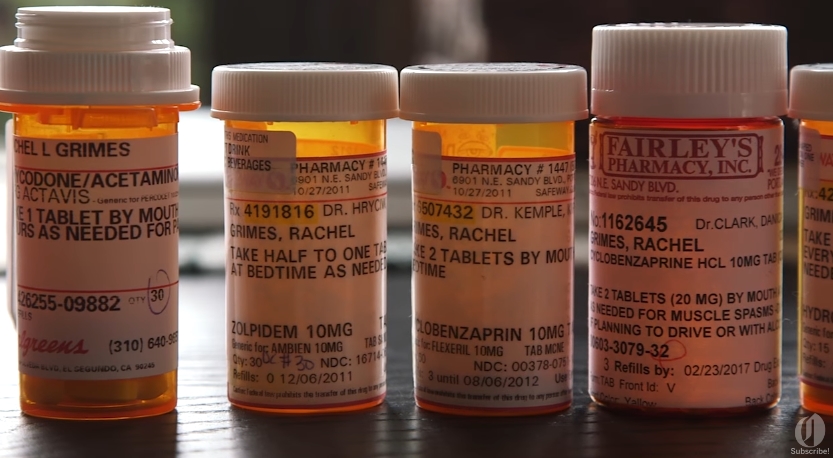
The PHQ-9 questionnaire has been used by doctors for twenty years. It contains only nine questions, and was developed by funding from major drug corporation Pfizer, a report on DailyMail.co.uk said. The company supplies commonly prescribed depression and anxiety medications, including Venlafaxine and Sertraline.
Through the questionnaire, patients are asked to rate their experiences of depression symptoms such as poor appetite, low energy, erratic sleep, and poor concentration levels, based on how often they’ve felt it — whether “on several days”, “nearly every day”, or the like. They are given scores based on their answers, and the total is then checked against a depression severity scale that goes from not depressed to severely depressed.
Many critics have found that the questionnaire lowers the standards for depression. They also criticized how doctors do not spend more time in conducting appropriate psychiatric interviews, saying that this could lead to a clinical depression diagnosis for a patient who is simply undergoing a stressful period in his or her life.
“GPs are very busy and they often don’t have time to do a full interview,” Dr. James Davies, co-founder of the Council for Evidence-Based Psychiatry, said in the DailyMail.co.uk report. “These forms have a very low criteria for anxiety and depression. Millions of people have filled them in and got medication, but did they know they were developed by Pfizer?”
While the discovery is troubling, other doctors deny a reliance on the PHQ-9 questionnaire. “They are used less and less by GPs, and where they are still used, scoring highly does not automatically lead to medication,” Professor Sir Simon Wessely, president of the Royal College of Psychiatrists, was quoted as saying in the report.
It would appear that depression is particularly vulnerable to overdiagnosis, with several studies suggesting that majority of patients who are diagnosed with depression fall short of meeting the official diagnostic criteria — and are dangerously given prescriptions for psychiatric medication as a result.
A study published in Psychotherapy and Psychomatics suggested just that, examining a sample of 5,639 participants who were diagnosed as depressed by clinicians in a non-hospital setting. The researcher, Ramin Mojtabai, conducted face-to-face interviews with the participants to re-evaluate them for major depressive disorder (MDD) based on criteria set in the Diagnostic and Statistical Manual (DSM). To qualify for MDD, participants must have experienced a major depressive episode for at least two weeks straight within a twelve-month period. A major depressive episode is characterized by a loss of interest in everyday activities, as well as other symptoms such as anxiety, feelings of emptiness, concentration problems, and appetite changes.
The study found that not even half of the participants — only 38.4 percent — were confirmed to have MDD in the re-evaluation. These results suggest that for the remaining 61.6 percent, the initial depression diagnosis was mistaken, though a majority of them had reported using antidepressants. The study concludes that overdiagnosis and overmedication for depression is all too common in the United States, and more stringent diagnostic and treatment practices are needed to ensure that all patients get the appropriate mental health help they need.
Sources include:
Tagged Under: Antidepressants, Big Pharma, depression, drug addiction, drug dependency, mental health, pharmaceutical drugs, psych drugs